Cardiac Arrhythmia Research. Simplified.
Discover our comprehensive ECG Analysis Suite.

Providing researchers immediate insight into ECG characteristics.
Track beat-to-beat changes in the cardiac depolarization pathways and get comprehensive dimensional and morphological characterization of all structures in your ECGs instantly.
Comprehensive wave, interval and segment measurements on all recorded ECGs.
Forget pens, paper and rulers. Invest your time where it truly matters.
Sophisticated algorithms provide visualization and characterization of the atrial activation.
High-resolution atrial signal acquisition, as easy and simple as a standard ECG recording.
Discover our complete Cardiac Arrhythmia research solution.
The power of high-resolution recording and cutting-edge data analysis for your cardiac arrhythmia research.
Originally designed to capture the unseen, the sensitivity of our system ensures no subtle information within the atrial nor the ventricular activation goes undetected.
All recorded free from any filters.
ECG Acquisition System
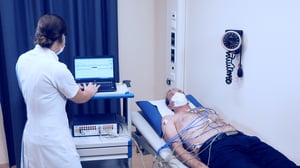
The system enables high-resolution recordings of the complete cardiac electrophysiological activation, through a wide range of options for atrial- or ventricular-optimized lead placements.
Recordings feature raw high-resolution signal, free from any set constraints on the recording length for optimal flexibility.
The High-Resolution Extended ECG Acquisition System provides tools for easy configuration and setup, data visualization, storage, and review and export of data. Signals and parameters can be checked in the display mode, stored to disk, reviewed in the offline mode or exported for further analysis.
The recording time of the ECG signals can be freely chosen by the user and there is no limitation in recording time. Raw signals can be filtered with specific high-pass, low-pass and notch filters. Recorded data is easily transferred to the ECG Analysis Suite.
YRS 100 Cardiac Amplifier has CE-Mark
CE-mark is pending for the Acquisition Software
![YRS100 Data Acquisition - lead selection[12]](https://www.yourrhythmics.com/hubfs/YRS100%20Data%20Acquisition%20-%20lead%20selection%5B12%5D.png)

.png)

A powerful analysis suite originally developed to handle the wealth of information in high-resolution quality recordings to provide the most comprehensive, validated, and research-proven characterization of the cardiac electrophysiological activity.
High-Resolution Extended ECG Analysis Suite
The High-Resolution Extended ECG Analysis Suite is an interactive environment for multimodal ECG data processing and analysis.
The ECG Analysis Suite is optimally suited for analysis of ECGs recorded with our High-Resolution Extended ECG Acquisition system, and ECGs recorded with other systems can be imported and analyzed as well.
For research only.
CE-mark is pending for the Analysis Suite
![Analysis SW Sinus Rhythm patient[17]](https://www.yourrhythmics.com/hubfs/Analysis%20SW%20Sinus%20Rhythm%20patient%5B17%5D.png)
![Analysis SW AF patient 2[22]](https://www.yourrhythmics.com/hubfs/Analysis%20SW%20AF%20patient%202%5B22%5D.png)
![Analysis SW AF patient 1[31]](https://www.yourrhythmics.com/hubfs/Analysis%20SW%20AF%20patient%201%5B31%5D.png)
Resources.
Researchers from the group of Prof. U. Schotten and Prof. H. Crijns at Maastricht University Medical Center extensively studied non-invasive characteristics of AF substrate complexity based on the ECG, leading to the development of our High-Resolution Extended ECG Solution.
How ECG-derived parameters quantifying AF complexity can improve AF classification, outcome prediction and optimize therapy for each individual AF patient is the object of many research publications.
Some publications authored by the Maastricht University group on this topic are presented below.
About YourRhythmics.
YourRhythmics was founded in 2016 as a spin-off of Maastricht University/Maastricht University Medical Center to support the group’s leading arrhythmia research with a system capable of characterizing the patients’ atrial substrate non-invasively through comprehensive analysis of the atrial electrophysiological contraction patterns on high-resolution atrial-optimized extended ECG.
YourRhythmics is conducting clinical trials and developing artifical intelligence algorithms to develop the very first in-clinic AF therapy decision support system offering optimal and personalized AF diagnosis and treatment outcome prediction, with the intention to increase AF therapy success rates and shorten the time frame from diagnosis to lasting symptom relief.
YourRhythmics operates from its office at Brightlands Maastricht Health Campus. Its solutions are developed in close cooperation with key researchers of the Maastricht University CARIM School for Cardiovascular Diseases, Maastricht Instruments BV, a product incubator for innovative medical devices, and AIM BV, a specialized manufacturer of electromechanical medical devices.


![Carim Uli Schotten.DSCF8510[14]-2](https://www.yourrhythmics.com/hs-fs/hubfs/Carim%20Uli%20Schotten.DSCF8510%5B14%5D-2.png?width=175&height=175&name=Carim%20Uli%20Schotten.DSCF8510%5B14%5D-2.png)